IMAGING THE EYE AND ORBIT
John R. Hesselink, MD, FACR
Inflammatory and neoplastic diseases of the orbit usually present with exophthalmos, pain, periorbital edema, visual impairment or ophthalmoplegia. The major imaging modalities for diagnosing orbital disease are ultrasound, MR, and CT. Orbital ultrasound is primarily in the domain of ophthalmology. Ultrasound is very good for evaluating ocular disease and for assessing the early changes of Graves' disease.

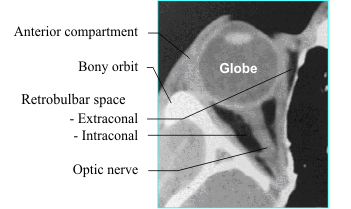
When considering orbital disease, it is helpful to localize the process to a compartment of the
orbit, both for purposes of differential diagnosis and for therapeutic planning. The orbital septum and
globe divide the orbit into anterior and
posterior compartments. The anterior
compartment consists of the lids, lacrimal
apparatus and anterior soft tissues. The
posterior compartment, also called the
retrobulbar space, is further divided into the
intraconal and extraconal spaces. The cone
consists of the extraocular muscles and an
envelope of fascia. The optic nerve is located
within the intraconal space. The bony orbit can
be considered the fourth compartment of the
orbit.
![]()
INFLAMMATION
The more common inflammatory diseases of the orbit include orbital cellulitis, Graves' disease and pseudotumor. Orbital cellulitis is an acute bacterial infection that most often represents extension of an infection from the paranasal sinuses or eyelid. The orbits are predisposed to infectious agents because they are surrounded by the paranasal sinuses, which are commonly infected. Secondly, the thin lamina papyracea offers little resistance to an aggressive process in the ethmoid sinuses. Finally, the veins of the face do not have valves and serve as another pathway for extension of inflammation into the orbit.
Cellulitis
Preseptal cellulitis appears as an area of increased density on CT scan, with swelling of the
anterior orbital tissues and obliteration of the fat planes. The fibrous orbital septum offers some
resistance to extension of the infection into the posterior compartment of the orbit. Often, the first
sign of involvement of the orbit is a slight increase in density of the orbital fat. This is followed by
development of more discrete densities as the infectious process progresses. In most cases, the
cellulitis is confined to the extraconal space but, if left untreated, it can enter the muscle cone and
intraconal space. The cellulitis, in turn, can lead to orbital abscess formation. On MR, orbital
cellulitis is hypointense on T1- and hyperintense on T2-weighted images. Fat-suppression MR
imaging in conjunction with gadolinium enhancement may be the most sensitive imaging method for
detecting early inflammatory disease of the orbit.
![]()
Extension of an ethmoiditis into the orbit usually begins as a subperiosteal abscess. This can be identified on CT scan as a thin layer of high density immediately lateral to the lamina papyracea.
Graves' Disease
Graves' disease is the most common cause of bilateral proptosis. Seventy percent of cases are
bilateral and symmetrical. There is a four-to-one female preponderance. The disease is characterized
by symmetrical swelling of the extraocular muscles. The medial and inferior rectus muscles are most
often involved. The muscle enlargement character-istically involves the body of the muscle, sparing
the tendinous attachment to the globe. In cases of unilateral involvement, other diseases must be
considered.
![]()
Pseudotumor

Orbital pseudotumor is a non-specific inflammation of orbital tissues. It tends to be unilateral and
accounts for 25% of all cases of unilateral exophthalmos. It can be remitting or chronic and
progressive. It may spontaneously regress or respond to steroids. It involves predominantly the
tissues immediately behind the globe.
![]() The scleral margin often appears thickened due to
inflammatory edema of the sclera and fluid within Tenon's space. Pseudotumor is an infiltrative
process and usually involves both the extraconal and
intraconal spaces. It appears on CT scan as areas of
soft tissue density with poorly defined margins.
The scleral margin often appears thickened due to
inflammatory edema of the sclera and fluid within Tenon's space. Pseudotumor is an infiltrative
process and usually involves both the extraconal and
intraconal spaces. It appears on CT scan as areas of
soft tissue density with poorly defined margins.
The earliest changes of pseudotumor may be subtle edema of the retrobulbar fat. MR imaging with fat suppression may be the most sensitive method for detecting these early changes. Orbital myositis refers to solitary involvement of one of the extraocular muscles, usually the inferior rectus. Sometimes, pseudotumor will appear as a discrete mass and simulate a neoplastic lesion. Lymphoma must be considered in these cases because benign pseudotumor may evolve to lymphoma.
Other Inflammatory Lesions
Sarcoidosis
This is a systemic granulomatous disease that rarely involves the orbit. It primarily affects the retrobulbar tissues and can mimic pseudotumor. The inflammatory process can extend along the optic nerve posteriorly through the optic canal to involve the chiasm and adjacent structures in the suprasellar cisterns.
Optic neuritis
Optic neuritis can result from any of the above inflammatory disorders, can occur as an isolated
inflammation, or may be a part of the spectrum of multiple sclerosis. Patients usually present with
decreased visual acuity. The imaging findings can be quite subtle, and CT and conventional MR pulse
sequences may be normal. Successful diagnosis often requires a fat suppression MR technique in
conjunction with either a T2-weighted sequence or a T1-weighted sequence and gadolinium
enhancement.
![]()
Mucormycosis
A fungal infection, mucormycosis is associated mostly with poorly controlled diabetes, but any immunocompromised patient is at increased risk for this opportunistic organism. The infection usually starts in the nasal cavity or paranasal sinuses and secondarily involves the orbit. Extension into the intracranial cavity can occur via the superior orbital fissure or the cribriform plate. The clinical picture and imaging features are often indistinguishable from any other orbital cellulitis.
ORBITAL TUMORS
Many tumors of the orbit have specific imaging features and, by correlating these features with the location within the orbit and age of the patient, one can often arrive at a limited differential and clearly suggest the most likely histology.
Optic Nerve Lesions
The list of causes of optic nerve enlargement is long, but the differential is usually between optic nerve glioma and optic sheath meningioma.
Optic gliomas
These tumors occur in children, most often in association with neurofibromatosis (NF 1) . They are slow-growing, nonaggressive, and follow a relatively benign course. Imaging studies usually show fusiform enlargement of the optic nerve. They can extend posteriorly through the optic canal to involve the optic chiasm. From there, they can involve either the opposite optic nerve or the optic tracts. Most optic gliomas enhance with contrast infusion, but the enhancement pattern is variable.
Optic nerve sheath meningiomas

As in the intracranial compartment, meningiomas of the orbit occur most commonly in
middle-aged females. They usually have a tubular appearance on CT or MR as opposed to the
fusiform or globular shape of optic
gliomas. Meningiomas enhance more
than gliomas and the "railroad track"
appearance is a characteristic feature.
Calcification within the lesion favors
a meningioma. Hyperostosis around
the optic canal is another sign for
meningioma.
![]()
Intraconal/Extraconal Tumors
Cavernous hemangiomas
They are one of the more
common orbital tumors in adults.
They are benign, well-encapsulated
lesions with wide vascular spaces.
They appear as high-absorption lesions on plain CT and demonstrate marked homogeneous contrast
enhancement. They have well-defined margins and are round or oval in shape.
![]() Most are found in
the intraconal space, lateral to the optic nerve. MR imaging displays nonspecific prolongation of both
T1 and T2. Their vascular nature is not apparent on MR because they are not high flow lesions.
Most are found in
the intraconal space, lateral to the optic nerve. MR imaging displays nonspecific prolongation of both
T1 and T2. Their vascular nature is not apparent on MR because they are not high flow lesions.
![]()
Lymphangiomas
Tumors of children and young adults, lymphangiomas often have poorly defined margins, and they
show little or no contrast enhancement. Although benign, they are infiltrative lesions and often
involve both the anterior and posterior compartments of the orbit. The cystic components are often
characteristic on MR, with multiple fluid levels of varying signal intensity.
![]() Since lymphangiomas are
characterized by slow, but relentless growth, expansion of the bony orbit can occur. Acute proptosis
may develop secondary to an upper respiratory tract infection or from intratumoral hemorrhage.
Since lymphangiomas are
characterized by slow, but relentless growth, expansion of the bony orbit can occur. Acute proptosis
may develop secondary to an upper respiratory tract infection or from intratumoral hemorrhage.
![]()
Lymphoma

Lymphoma is relatively uncommon in the orbit, and is
usually associated with pseudotumor or systemic lymphoma.
The most common sites are the conjunctiva and lacrimal
gland. They tend to be homogeneous lesions with relatively
well-defined margins. They can be more aggressive and
invade adjacent sinus compartments.
![]()
Other tumors
Rhabdomyosarcoma is the most common primary malignant orbital tumor of childhood. It is a very aggressive tumor and often shows extensive destruction. Teratomas of the orbit are rare, but are characterized by areas of calcification and fat density.
Tumors of the Eyelid and Preseptal Space
Tumors of the anterior compartment readily extend posteriorly into the extraconal space. Basal
cell carcinoma accounts for 80% of eyelid neoplasms. Other histologies include squamous cell and
sebaceous cell carcinomas and adenocarcinoma.
![]()
Lacrimal Region
If a mass is found in the superolateral quadrant of the orbit, one should consider dermoid cysts and lacrimal gland masses. Dermoid cysts arise from epithelial rests found at sutural sites within the orbit. They often have cystic centers with variable enhancement of the perimeter. The cyst contents are frequently low density on CT and exhibit T1 shortening on MR, and a fluid level may be present.
Fifty percent of lacrimal gland tumors are pleomorphic adenomas and the other half are malignant. The malignant category includes predominantly adenocystic, pleomorphic, and mucoepidermoid carcinoma. The lacrimal tumors have few distinguishing imaging features, showing mostly a homogeneous character and moderate contrast enhancement. Poorly defined margins with bone destruction suggests a malignancy, but even the malignant lesions can be relatively well-defined.
VASCULAR LESIONS
An important vascular lesion to consider in the orbit is orbital varix. They appear as fusiform or globular densities on the CT scan and enhance brightly with contrast. A mixture of flow void and flow enhancement may be seen on MR. By increasing venous pressure with a Valsalva maneuver, the varix may increase in size, confirming the diagnosis.
Arteriovenous malformations of the orbit are rare as isolated lesions and are usually associated with intracranial AV malformations. Also, a carotid-cavernous fistula often produces profound dilatation of the intraorbital venous structures. The Wyburn-Mason syndrome consists of an AV malformation extending from the midbrain along the anterior visual pathways to the orbit and retina. Retinal angiomatosis is a feature of von Hippel-Lindau disease. The extraocular vascular lesions usually present with orbital congestion and proptosis. Those involving the globe may present with visual deficits or hemorrhage. Serpiginous areas of flow-void often provide the clue for diagnosis on MR scans.
OCULAR LESIONS
Retinoblastoma
Retinoblastoma is the most common intraocular malignant tumor of childhood. The disease
presents during the first two years of life. Only 10% of cases are inherited as an autosomal dominant
trait; the rest result from sporadic mutations of chromosome 13. About 30% are bilateral. On CT
scan, they appear as high-density areas arising from the retina. Calcifications are common and, when
present in a child, should suggest retinoblastoma. Retinal detachment is invariably present, and the
subretinal fluid can be readily identified on MR images. Retinoblastoma must be distinguished from
benign causes of leukocoria.
![]()
Congenital Lesions
In persistent hyperplastic primary vitreous (PHPV), the primary vitreous fails to involute
before birth and becomes hyperplastic.
![]() Coats' disease is an exudative retinopathy that fills the
subretinal space with a lipoproteinaceous fluid. Calcification is uncommon in the "pseudogliomas"
but the specific diagnoses can not always be made from the CT or MR alone. Microphthalmos is
associated with PHPV.
Coats' disease is an exudative retinopathy that fills the
subretinal space with a lipoproteinaceous fluid. Calcification is uncommon in the "pseudogliomas"
but the specific diagnoses can not always be made from the CT or MR alone. Microphthalmos is
associated with PHPV.
![]()
Anophthalmos is due to failure of development of the optic vesicle, and patients are invariably blind in the eye. It is often bilateral and may be associated with an optic vesicle cyst.
Melanoma
This malignant tumor of the choroid occurs in the sixth and seventh decades of life. They are
almost always single and uniocular, and most arise from preexisting nevi in the choroid. Melanomas
are aggressive tumors, invading along the choroid, into the vitreous, and through the sclera into the
optic nerve and retrobulbar space. They are high density on CT and do not calcify. Compared to the
vitreous, they are high signal on T1-weighted images and low signal on T2-weighted images.
Subretinal effusion is very common.
![]()
The primary differential for melanoma is choroidal metastasis. Breast and lung carcinomas are the most common primaries, followed by gastrointestinal and genitourinary tumors. The primary may not be known at the time of presentation in as high as 50% of ocular metastases. Carcinomas usually exhibit moderate signal on T1-weighted images and high signal on T2-weighted images.
Benign Lesions
Optic nerve drusen represents cellular accretions of hyaline-like material in the optic disk. They are bilateral in 73% and frequently calcify. Many are asymptomatic, but arcuate visual field defects may be present. CT scan shows discrete rounded high densities confined to the optic disk surface. Choroidal osteomas can be idiopathic or may develop within a degenerated choroidal hemangioma or an inflammatory scar. They are usually located near the optic disk. If they involve the area of the fovea, vision will be affected. Colobomas are caused by a defect in the sclera, allowing ocular contents to herniate posteriorly into the retrobulbar space. Most are congenital, but some are secondary to an inflammatory process that severely weakens the sclera. The optic nerve head is often involved by congenital colobomas.
SUMMARY
In summary, for optic nerve lesions, consider optic nerve glioma or optic sheath meningioma. If the CT or MR scan shows enlargement of the extraocular muscles, think of Graves' disease or pseudotumor. A well- defined contrast-enhancing mass in the retrobulbar region is most likely a cavernous hemangioma. For an intraocular lesion, consider retinoblastoma or melanoma. In all cases, remember to ask for the patient's age.
REFERENCES