THE TEMPORAL LOBE & LIMBIC SYSTEM
John R. Hesselink, MD, FACR
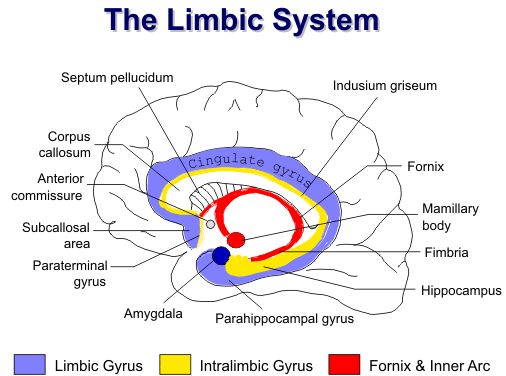
The limbic lobe is a complex set of three C-shaped structures containing both gray and white matter. It lies deep within the brain and includes portions of all the lobes of the cerebral hemispheres. A myriad of fiber tracts connect the limbic lobe with numerous deep nuclei and the olfactory apparatus to form the limbic system. Phylogenetically, the limbic system is one of the more primitive parts of the brain. It has a central role in memory, learning, emotion, neuroendocrine function, and autonomic activities. Clinical conditions involving the limbic system include epilepsy, congenital syndromes, dementias, and various psychiatric disorders.

ANATOMY
Limbic System
The outer arc of the limbic system (also called the limbic gyrus) includes the subcallosal area, the
cingulate gyrus, the isthmus of the cingulate gyrus, and the parahippocampal gyrus, including the
uncus and subiculum. The subcallosal area includes a cluster of small septal nuclei that lie
immediately anterior to the paraterminal gyrus and anterior commissure. The septal nuclei receive
input from multiple midbrain nuclei, the substantia nigra, the CA1 region of the cornu ammonis, the
subiculum, amygdala, lateral hypothalamus, cingulate gyrus, and mamillary bodies. Efferent fibers
project to the entire hippocampal formation, the habenula, hypothalamus, thalamus, amygdala,
mamillary bodies and the cerebral cortex.
![]()
The middle arc (also referred to as Broca’s intralimbic gyrus) consists of the paraterminal gyrus, the indusium griseum, and the hippocampus. The paraterminal gyrus is wedged between the septal nuclei and the anterior commissure. Posterior to the anterior commissure is the hypothalamus. The indusium griseum, extending from the paraterminal gyrus, consists of gray matter and white matter tracts named the medial and lateral longitudinal stria. The indusium griseum is closely applied to the superior surface of the corpus callosum. Posteriorly, it courses around the splenium and inferiorly merges with the tail of the hippocampus.
The mamillary bodies, fornix, alveus and fimbria form the inner arc. The alveus and fimbria are
the major efferent fibers tracts of the hippocampus. Posteriorly, the fimbria form the crura of the
fornix that continue upward deep to the splenium of the corpus callosum. As the two crura converge,
a thin triangular sheet of fibers passes to the opposite side to form the commissure of the fornix. The
crura merge as the body of the fornix, which continues forward along the inferior edge of the septum
pellucidum and roof of the third ventricle. At the foramen of Monroe, the fornix divides into two
columns which course inferiorly. Just superior to the anterior commissure, the columns divide into
pre- and postcommissural tracts. The precommissural fibers connect to the septal nuclei and anterior
hypothalamic nuclei. The postcommissural fibers continue inferiorly to end in the mamillary bodies.
![]()
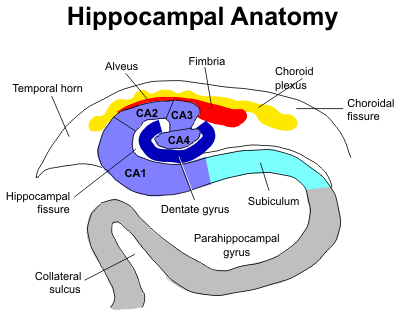
Hippocampus
The hippocampus is a part of the middle arc of the limbic sys tem. It is located in the medial temporal lobe inferior to the choroidal fissure and temporal horn. In the sagittal plane the hippocampus is a club-shaped structure divided into three parts: head, body, and tail. The more anterior head is marked by digita tions and is also called the pes hippocampus. The body is more cylindrical in shape, and the tail tapers posteriorly.
The gray matter of the hippo
campus is an extension of the
subiculum of the parahippo-
campal gyrus. In coronal plane
the hippocampus and parahippocampal gyrus form an S-shaped configuration. The hippocampus
itself consists of two interlocking C-shaped structures: the cornu ammonis and the dentate gyrus.
Histologically, the hippocampus is further divided into four sections: CA1 to CA4.
![]()
The amygdala is positioned directly anterior to the pes hippocampus and above the tip of the
temporal horn. The alveus and fimbria, white matter tracts along the superior surface of the
hippocampus, continue posteriorly as the fornix and serve as the major efferent pathways to the rest
of the brain.
![]()
FUNCTION
The limbic system is associated with emotion and motivation. The amygdala is known to attach emotional significance to sensory input. Olfactory stimuli enter the limbic loops via the entorhinal cortex of the parahippocampal gyrus. The limbic system has a direct influence on neuroendocrine, autonomic, and behavior mechanisms, and it also has a role in functions such as fight or flight, homeostasis, self-maintenance, appetite, and sexuality. As noted above, structures of the limbic system are highly interconnected with the rest of the brain, and they likely form a gateway for communication between the cerebral cortex and the hypothalamus. This gateway allows for cognitive processes to modify the affect of the limbic system on hypothalamic functions.
The hippocampus, fornix, and mamillary bodies have an integral role in memory and learning.
Much of what we know about temporal lobe function comes from patients with temporal lobectomies
for tumors or intractable seizures. Impaired verbal memory is associated with left anterior temporal
lobectomies, whereas right temporal lobectomy may result in visual/spatial memory disturbances. The
degree of impairment is directly related to the age of the patient. Young children have considerable
plasticity, allowing for other areas of the brain to take over the function of the resected portion. The
decrease in memory function after temporal lobectomy is directly related to the amount of medial
temporal lobe resected and the level of memory function prior to surgery (the more you have, the
more you stand to lose), and it is inversely related to the degree of hippocampal sclerosis of the
resected lobe.
![]()
EPILEPSY
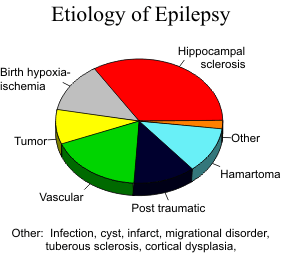
Epilepsy is defined as recurrent unprovoked seizures characterized by transient disturbances in mentation and movement. It is caused by exces sive abnormal electrical activity in the brain. Epilepsy can be partial or generalized. Partial epilepsy is further divided into partial simple or partial complex, depending on whether or not the seizures are associated with loss of consciousness. About 20 to 25% of epilepsy is refractory to medical therapy and is referred to as “intractable epilepsy.” Temporal lobe epilepsy is the most common epilepsy in adults and is most often caused by hippocampal sclerosis
Mesial Temporal (Hippocampal) Sclerosis
Hippocampal sclerosis is characterized by neuronal loss and gliosis with secondary atrophy and
sclerosis. With additional involvement of the amygdala and parahippocampal gyrus, the term mesial
temporal sclerosis (MTS) is appropriate. The etiology is not certain, however, febrile seizures during
infancy have been implicated in a number of series. The neuronal loss and gliosis occurs in all
segments of the cornu ammonis and dentate gyrus, but it is most prominent in the CA1 region with
relative sparing of the CA2 segment. The involvement is usually most prominent in the body of the
hippocampus, followed by the tail and head. Bilateral disease is seen in 10-15% of cases. With
unilateral hippocampal sclerosis, anterior temporal lobe resection cures the epilepsy in 90% of
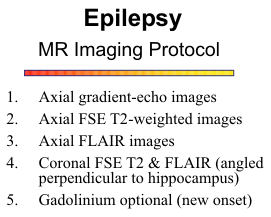
The most common findings on MR imaging are
hippocampal atrophy and hyperintensity on T2-
weighted images. FLAIR images are most sensitive
for detecting the abnormal hyperintensity, however,
high signals from the choroid plexus or CSF flow
artifacts in the temporal horn can be confusing.
![]()
With high resolution imaging, loss of the normal
internal architecture of the hippocampus can be
identified.
![]() MR imaging is reported to be 80-90%
sensitive for detecting hippocampal sclerosis. Quan
titative volume measurements from thin-section 3D
MR sequences can increase the sensitivity.
MR imaging is reported to be 80-90%
sensitive for detecting hippocampal sclerosis. Quan
titative volume measurements from thin-section 3D
MR sequences can increase the sensitivity.
![]() Associ
ated findings include atrophy of the parahippocampal gyrus, decreased volume of the adjacent white
matter, and temporal horn dilatation. Since the fornix is the primary efferent pathway from the
hippocampus, severe damage to the hippocampal neurons can result in atrophy of the ipsilateral
fornix.
Associ
ated findings include atrophy of the parahippocampal gyrus, decreased volume of the adjacent white
matter, and temporal horn dilatation. Since the fornix is the primary efferent pathway from the
hippocampus, severe damage to the hippocampal neurons can result in atrophy of the ipsilateral
fornix.
![]() Gadolinium enhancement is not helpful for the diagnosis of hippocampal sclerosis.
Gadolinium enhancement is not helpful for the diagnosis of hippocampal sclerosis.
Neoplasia
Gliomas are malignant tumors of the glial cells of the brain and account for 30-40% of all primary
intracranial tumors. Astrocytomas are graded according to their histologic appearance. The lower
grades are well-differentiated and slow-growing; the higher grade glioblastoma is highly malignant
and grows very rapidly. Oligodendrogliomas are the most benign of the gliomas. Calcification is
common, and they occur predominantly in the frontal lobes. The mixed neuronal and glial tumors,
such as the ganglioglioma and dysembryoplastic neuroepithelial tumors (DNET), are found mostly
in children and young adults. They are slow-growing and are found predominantly in the temporal
lobes and around the third ventricle. Intratumoral cysts and calcification are common.
![]()
The common signal characteristics of gliomas include high signal intensity on T2-weighted images and low signal on T1-weighted images. Gliomas infiltrate along white matter fiber tracts and have poorly defined margins. The higher grade gliomas, particularly glioblastomas, appear heterogeneous due to central necrosis with cellular debris, fluid, and hemorrhage. Peritumoral edema and mass effect are common. Most exhibit irregular ring-enhancement. The lower grade astrocytomas tend to be more homogeneous without central necrosis. Large cystic components may be present. The cysts have smooth walls, and the fluid is of uniform signal, to distinguish them from necrosis. Enhancement is variable, depending on the integrity of the blood-brain barrier.
Metastatic disease needs to be considered when multiple lesions are present. Occasionally, lym-phoma will present in the medial temporal lobe.
It is not uncommon to find an incidental arachnoid cyst in the choroidal fissure. They are generally small and of no clinical significance. Also, an epidermoid tumor in the adjacent basal cisterns may extend into the choroid fissure.
Vascular Lesions
Most cavernous angiomas are asymptomatic, but they may be a source of temporal lobe seizures.
They invariably contain hemosiderin from chronic hemorrhage and are distinctly hypointense on T2-weighted MR images. Lesion margins are "fuzzy" due to the magnetic susceptibility effect of the
hemosiderin. Calcification is often present. Mild enhancement can be obscured by the hemosiderin.
![]()
One-half of patients with arteriovenous malformations present with seizures. CT features of an AV malformation on plain scan include a high- absorption irregular mass with large feeding arteries and draining veins, focal areas of calcification and no surrounding edema or mass effect. The contrast scan shows serpiginous enhancement with prominent arteries and veins. Due to the rapidly flowing blood from these lesions, a flow void is observed on MR scan. As a result, the characteristic feeding arteries and draining veins can be imaged without any injection of contrast material.
Infection
Any CNS inflammatory condition can involve the temporal lobe. Herpes simplex is one organism
that has an affinity for the medial temporal lobes. Herpes simplex is the commonest and gravest form
of acute encephalitis with a 30-70% fatality rate and an equally high morbidity rate. It is almost
always caused by Type 1 virus except in neonates where Type 2 predominates. Symptoms may
reflect the propensity to involve the inferomedial frontal and temporal lobes - hallucinations, seizures,
personality changes and aphasia. Early involvement of the limbic system and temporal lobes is
characteristic of herpes simplex encephalitis. The cortical abnormalities are first noted as ill-defined
areas of high signal on T2-weighted scans, usually beginning unilaterally but progressing to become
bilateral. Edema, mass effect and gyral enhancement may also be present.
![]()
CNS tuberculosis usually presents as a meningitis, but hematogenous spread can result in cerebral tuberculomas. Mature tuberculomas are T2 hypointense. Central necrosis in some lesions results in a T2-bright core with a low signal intensity rim.
Neurocysticercosis is the most frequently encountered parasitic infestation of the CNS. Humans are accidental hosts for the larval stage of Taenia Solium, the pork tapeworm. Seizures are a common clinical presentation. Parenchymal lesions consist of small cysts, large cysts and calcified lesions. The smoothly marginated cysts are uniformly hyperintense on T2-weighted images. The presence of a mural nodule or a T2-hypointense rim in encapsulated lesions may correlate with larval death. Visualization of calcified lesions has been variable with MR; overall there is an advantage for CT in this regard.
Trauma
The anterior temporal lobe is susceptible to traumatic injury. Deceleration forces compress the cortex against the protruding edge of the sphenoid wing. Brain contusion results in encephalomalacia and gliosis that can lead to posttraumatic epilepsy. Intracranial mass effect can result in major shifting of brain structures that can damage the temporal lobe. With downward pressure, the uncus of the temporal lobe is displaced medially and inferiorly through the tentorial incisura. The combination of compression against the sharp edge of the tentorium and compromise of the blood supply to the medial temporal lobe can result in significant damage.
Developmental Lesions
Epilepsy is commonly associated with developmental anomalies, particularly disorders of neuronal
migration and cortical organization. This long list of disorders includes lissencephaly, pachygyria,
polymicrogyria, cortical dysplasia, schizencephaly, gray matter heterotopia, microcephaly, and
megalencephaly. All are characterized by a disordered cortical architecture, abnormal deformed
neurons, and apparent loss of inhibitory neurons.
![]()
Two neurocutaneous syndromes are associated with epilepsy in 80% of cases. The classic features of tuberous sclerosis include autosomal dominant inheritance and the clinical triad of seizures, adenoma sebaceum, and mental retardation. Multiple nodules or tubers are distributed throughout the cerebral cortex and subependymal regions. Histologically, the subpial regions of the involved cortex disclose gliosis and proliferating astrocytes that are large and bizarre with abundant processes.
Sturge-Weber syndrome consists of a facial vascular nevus and leptomeningeal angiomatosis.
Clinical features include seizures, hemiparesis, and hemianopsia, reflecting the unilateral cortical
involvement. The involved cortex is frequently atrophic with neuronal loss and gliosis. Cortical
calcification and pial enhancement are common imaging findings.
![]()
DISEASES RELATED TO THE LIMBIC SYSTEM
Developmental abnormalities
The limbic system is directly involved by congenital abnormalities of ventral induction, namely holoprosencephaly, and septo-optic dysplasia. Clinically, alobar holoprosencephaly displays microcephaly, hypotelorism, and cyclopia. The brain is grossly malformed with a monoventricle, fused thalami, and absent interhemispheric fissure, falx, septum pellucidum, and corpus callosum. All 3 arcs of the limbic system are affected, and the septal nuclei and hypothalamus are often hypoplastic. Semilobar and lobar holoprosencephaly have lesser degrees of abnormality.
Septo-optic dysplasia is caused by failure of the optic vesicle and commissural plate. The septum pellucidum is absent and the optic nerves and chiasm are hypoplastic. Hypoplasia of the hypothalamus, pituitary gland, and septal nuclei are other features.
Limbic encephalitis
Limbic encephalitis is a paraneoplastic syndrome that has been reported with carcinoma of the
lung, breast, and some other primaries. The mechanism of disease is not known but it manifests as
an encephalitis that primarily involves the hippocampus, amygdala, cingulate gyrus, insula, and
orbital-frontal cortex. Afflicted patients develop subacute onset of memory loss, dementia,
involuntary movements, and ataxia.
![]()

Dementia
Degenerative changes in the limbic system likely have a role in the genesis of neurodegenerative diseases, particularly Pick’s disease and Alzheimer’s disease. The frontal and temporal lobes are predominantly affected by Pick’s disease. Marked atrophy is also found in the limbic system, most notably the dentate gyrus and hippocampus.
Alzheimer’s disease is a chronic pro
gressive dementia of unknown origin.
Early on, patients develop memory impair
ment which eventually progresses to global
intellectual dysfunction. Brain atrophy is
more diffuse in Alzheimer’s disease. Senile
plaques and neurofibrillary tangles are
dispersed throughout the cerebral cortex
and basal ganglia, but the hippocampus and amygdala are often severely involved. Secondary atrophy
of the fornix can be seen in chronic cases. Hippocampal atrophy may be a prominent feature on
imaging studies, but the finding is nonspecific and the diagnosis of Alzheimer’s disease requires
clinical correlation. Volumetric measurements of the amygdala and hippocampus as a unit may be
helpful for distinguishing patients with early Alzheimer’s disease.
![]()
Neuropsychiatric Disorders
Links to the limbic system are suspected for several psychiatric disorders, but the structural
alterations are subtle and generally require volumetric analysis for detection. The most studied
diseases are schizophrenia and bipolar (affective) disorder. The limbic system has also been
implicated in psychopathic and amnestic disorders, but no specific imaging criteria have been
developed.
Anxiety disorders include stress disorders, phobias, and panic attacks. The amygdala attaches
emotional significance to sensory input. Functional MR studies have revealed overactivity of the
amygdala during facial recognition tasks. Also, neuroscientists have identified a fear circuitry,
whereby the amygdala modulates neural circuitry in orbital, ventral and prefrontal cortex, the anterior
cingulate and the entorhinal cortex. Another theory is that anxiety disorders result from failure of the
anterior cingulate and hippocampus to modulate the activity of the amygdala.
![]()
Multiple studies of patients with schizophrenia have shown ventricular enlargement and reduced
limbic volumes. Additional findings include decreased size of hippocampus, decreased thalamic
volumes, decreased amygdala response during facial recognition tasks (fMRI), and decreased activity
in dorsolateral prefrontal cortex (PET). Of interest, the presence of a cavum septum pellucidum,
cavum vergae, and dysgenesis of the corpus callosum have been associated with schizophrenia,
suggesting possible disruption of afferent and efferent pathways to and from the septal area.
![]()
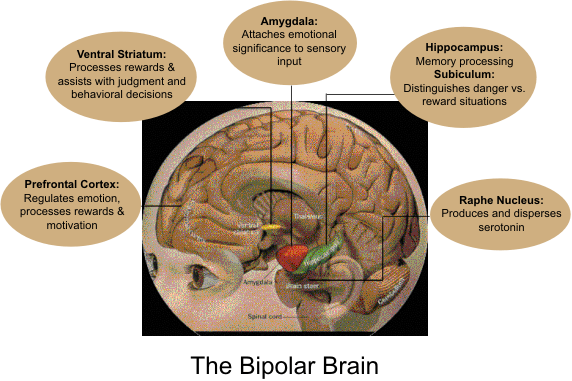
Bipolar or affective disorder features severe depression alternating with episodes of hyperactivity. Patients have defective regulation of emotions, and they have difficulty with judgment and behavioral decisions. The most popular theory is that a deficiency of serotonin is the primary cause of the disorder. Serotonin is normally produced in the raphe nucleus in the midbrain and upper pons and is distributed to the rest of the brain. Ventriculomegaly is observed in affective disorders, but the finding is nonspecific. Reductions in volume of the frontal lobes, basal ganglia, amygdala, and hippocampus have also been reported. Functional studies have revealed decreased activity in the prefrontal cortex and anterior cingulate gyrus.
Psychopathic disorders are characterized by aggressive and impulsive behavior. Patients are thought to have deficits in informational and emotional processing. A likely root cause is malfunction of neural circuits in the prefrontal and temporal-limbic regions.
REFERENCES