Evaluation of the head and neck has developed significantly with the
advent of CT and MRI. These modalities have greatly complimented the physical
and endoscopic examinations by revealing possible blind areas such as nonpalpable
adenopathy, cartilage invasion, bone marrow invasion, contralateral involvement,
and distant metastases. MRI has some major advantages over CT. Superior
soft tissue contrast is possible with MRI leading to better definition between
tumor and adjacent structures. Multiplanar imaging can be extremely helpful
in appreciating and confirming the extent of disease. There is a lack of
beam hardening artifacts which are encountered with CT when dental fillings
are present. In patients who can not tolerate intravenous iodine contrast,
MRI with gadolinium can still be performed. In order to optimally evaluate
the head and neck for pathological processes, one must first have a clear
understanding of the anatomy of the head and neck.
Anatomical Considerations:
In addition to understanding basic anatomical structures such as the
tongue, the tonsilar fossa, the epiglottis, the paranasal sinuses, the nasal
cavity, and the larynx, one must also be aware of certain anatomical spaces
which are delineated by fascial planes. These anatomical spaces throughout
the head and neck represent potential vertical highways for tumor spread
of pathological processes.
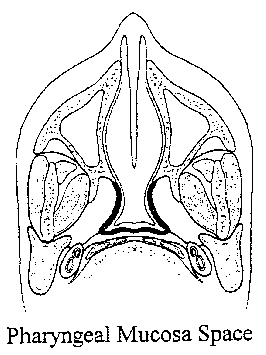
Pharyngeal Mucosal Space:
This space is located very superficially along the pharyngeal mucosal
walls. It includes the mucosa of the pharynx, Waldeyer's ring, the cartilaginous
eustachian tube, the pharyngobasilar fascia, the levator and constrictor
muscles. Common tumors seen in this space would include squamous cell cancer,
lymphoma, and sometimes adenocarcinoma, adenoid cystic carcinoma, and juvenile
angiofibromas. Thornwaldt cysts and mucous retention cysts can also be found
along this space. It represents a very superficial layer for which tumors
often will develop before they spread to deeper layers. This space is probably
less important from an imaging standpoint than the deeper spaces as an endoscopist
can usually detect tumor spread along this space without difficulty.
* Most superficial layer includes the pharyngeal mucosa,
Waldeyer's Ring, eustachian tube, constrictor and levator muscles. * Common masses:
|

Parapharyngeal Space:
This is an important vertical highway which extends from the skull base
to the hyoid bone. Tumors that may arise along the pharyngeal mucosal space
such as squamous cell cancer of the tonsilar fossa, can spread to the next
deeper layer which is often the parapharyngeal space. Once in the parapharyngeal
space, it can spread in a vertical manner very quickly. The parapharyngeal
space contains primarily fat, branches of the trigeminal nerves, and the
pterygoid veins. Lesions that are frequently encountered in this space include
metastatic lesions from squamous cell cancer, particularly from the base
of the tongue, tonsilar fossa, and larynx. Salivary gland tumors may also
be encountered in this space as a result of direct extension. Branchial
cleft cysts can develop or cross through this space. Lipomas may arise denovo
from the fat within this space. Infections can also run rampant in this
space in a very rapid manner.
* Fat filled space with some twigs of the fifth nerve and pterygoid veins. * Extends from skull base down to the hyoid bone. * METS (squamous cell cancer), infection, lipomas, pleomorphic adenomas, branchial cleft cysts. |

Carotid Space:
This is another major highway through which tumors can race vertically
up and down from the skull base down to the aortic arch., This space includes
the extracranial carotid artery, the jugular vein, portions of cranial nerves
9 through 11, the internal jugular chain of nodes. Metastatic lesions from
squamous cell cancer can frequently be found in this space. Popular sites
of origin for squamous cell cancer to invade the carotid space include the
larynx, the tongue base, the tonsilar fossa, and the nasal pharynx. Other
lesions that can be found in the carotid space would include neurofibromas,
Schwannomas, paragangliomas, and lymphomas. Infections which may be harbored,
particularly in the internal jugular nodes, can also be detected in the
carotid space. Involvement of the carotid space may be an indicator for
nonresectability, particularly if the carotid artery is encased.
* Includes carotid artery, internal jugular vein, cranial nerves 9-11, internal. jugular chain of nodes. * Extends from skull base down to aortic arch. Major verticle highway. * Common tumors:
* Encasement of the carotid artery may mean inoperability. |

Prevertebral Space:
This is a complex space which is enveloped by a deep layer of cervical fascia. It includes not only the longus coli muscles, but also the paraspinous muscles, the vertebra, the vertebral artery, and the spinal cord. Metastatic lesions to the prevertebral space as well as to the carotid space can potentially determine inoperability. For that reason, close scrutiny of tumor extension to the prevertebral space is very important. Common neoplasms that are found in the prevertebral space include metastatic lesions particularly from squamous cell carcinoma of the tonsilar fossa, the nasopharynx, the larynx, and the base of the tongue. Chordomas can also be found in this space. Infections from vertebral osteomyelitis and/or prevertebral abscesses may also be encountered in this area.
* Longus colli muscles, spine, spinal cord, vertebral bodies, paraspinus muscles. * METS involving the prevertebral space may also mean inoperability as
a tumor-free margin can not be obtained. * Common masses
|

Submandibular Space:
This space contains the submandibular gland, submandibular nodes, and portions of the facial vein and artery as well as the inferior loop of cranial nerve 7. Squamous cell cancer from the base of the tongue and floor of the mouth can extend into this space. Other types of tumors involving this space may include the variety of salivary gland tumors ranging from mucoepidermoid to adenoid cystic to pleomorphic adenomas.
* Includes submandibular gland, nodes, facial vein nerve and artery. * Malignancies:
* Benign:
|

This space contains the parotid gland and the parotid segment of cranial nerve 7. The retromandibular vein in external carotid arteries also pass through this space. Common tumors in this location would include pleomorphic adenomas, Warthin's tumors, mucoepidermoid carcinomas, adenoid cystic carcinomas, hemangiomas, and squamous cell carcinomas.
* Includes parotid gland, cranial nerve 7, external carotid artery, retromandibular vein. * Common Tumors:
|

Masticator Space:
This space contains the muscles of mastication. These include the masticator, temporalis, the medial and lateral pterygoids. Metastatic extensions of squamous cell carcinoma, particularly from the floor of the mouth, tonsilar fossa, and nasopharynx can be found extending into this space. Salivary gland tumors can also extend into this space. If neoplasm is discovered in this space, one should check for extension to the side of the skull as the masticator space extends very high into the suprazygomatic region along the temporalis muscle. One should also check for possible perineural spread, particularly along the course of the mandibular division of cranial nerve 5. Lymphomas and hemangiomas as well as cellulitis or abscesses can also be found in this compartment.
* Masseter, medial lateral pterygoid muscles, temporalis. * Common Masses:
* Warning checks:
|

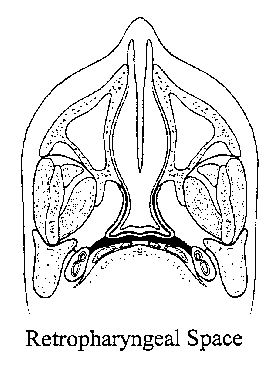
Retropharyngeal Space:
This is a posterior potential midline space which can also present a
major highway extending cephalad to the skull base or caudad down to approximately
the T3 level. Common lesions which can involve this space would include
lymphomas, metastatic tumors, particularly from squamous cell cancer, and
infections.
* Posterior mid-line potential space extending from skull base to approximately T3. * Common Masses:
|
Lymph Node Evaluation:
We consider nodes to be suspicious for metastatic disease by size. In
the jugular digastric region (levels 1, 2, and 3 or submandibular and upper
internal jugular chain) nodes that are larger than 1.5
centimeters in diameter should be considered very suspicious for metastasis.
Nodes in all other levels of the neck exceeding 1 centimeter in size, should
be considered abnormal. Nodes with necrosis should also be considered abnormal
regardless of size. One should also pay attention to nodes that have ill
defined borders as there may be extracapsular extension with infiltration
of the surrounding fat planes or encasement of vessels such as the carotid.
Abnormal supraclavicular nodes may represent metastasis from any source, but lung, breast, and esophagus are particularly common sources. Abnormal adenopathy along the inferior jugular chain may be due to metastatic disease from the supraglottic larynx, esophagus, or thyroid. Abnormal adenopathy in the midjugular chain may be related to
metastasis from tongue, pharynx, or supraglottic larynx cancers. Those
along the jugular digastric region are often related to metastasis from
the pharynx, tonsil, tonsilar fossa, tongue, parotid gland, or supraglottic
larynx. Submandibular adenopathy may be related to metastasis from adjacent
skin, submaxillary gland, or base of the tongue. Posterior triangle nodes
may be seen with metastasis from the pharynx, the nasopharynx, tongue base,
tonsilar fossa, or thyroid.
* Suspicious for malignancy if greater than 1.5 centimeters in juglo-digastric region; 1 centimeter or greater elsewhere. * Central necrosis makes lymph nodes suspicious for malignancy regardless
of size. * Check for extra capsular extension as this carries a very poor prognosis. |
Coronal CT is usually the most functional projection for evaluating the paranasal sinuses. The osteomeatal complex represents a common drainage point for the anterior sinuses (frontal, ethnoid, and maxillary). A lesion placed at the osteomeatal complex can strategically obstruct the anterior sinuses.
Osteomeatal Complex: (Strategic point which a lesion
can obstruct the anterior sinuses.)
|
Inflammatory and/or allergic processes are usually seen as areas of mucoperiosteal
thickening, fluid or airfluid levels filling the paranasal sinuses. In severe
or complicated cases, bone changes (erosion or thickening) may be present.
A mucus retention cyst represents an obstructed gland. It is usually
seen as a rounded soft tissue mass attached to the wall of a sinus.
A mucocele is an obstructed sinus. Bone expansion can be present with
mucoceles.
* Polyps: Inflammatory or allergic etiology. * Papilloma:
|
Malignancies that affect the paranasal sinuses include squamous cell
carcinoma, non-hodgkins lymphoma, and salivary malignancies.
Nasopharyngeal carcinoma tends to have a predilection for the fossa of
Rosenmueller and therefore often presents with unilateral otitismedia or
unilateral mastoiditis in adults. This tumor likes to spread along the spinal
accessory chain of nodes and the suspicious node in the posterior triangle
may therefore alert one to the presence of nasopharyngeal carcinoma. Likewise,
the finding of unilateral otitismedia and/or mastoiditis in an adult, should
direct one to the nasopharynx to be sure that there is not an early nasopharyngeal
cancer lurking.
* Warning sign: Unilateral otitis media/mastoiditis in adult. * Arises at fossa of Rosenmuller. * May metastasize to spinal accessory nodes in posterior triangle. |
Non-Hodgkin's lymphoma is the second most common nasopharyngeal malignancy.
Most are histiocytic or lymphocytic types of lymphomas. Hodgkin's lymphoma
is very uncommon in the head and neck. Cervical lymph node involvement is
common in non-Hodgkin's lymphomas of the head and neck and involvement of
Waldeyer's ring is often seen. These tumors tend to be very bulky and can
easily cross fascial planes.
* Bulky masses. * Cross fascial plains easily. * May be accompanied by large cervical nodes. * May have thickening of Waldeyer's Ring. * Tends to be destructive rather than blastic. * May involve a solitary gland such as the thyroid gland with or with out adjacent adenopathy and may arise very rapidly. |
Other malignancies that occur in the nasopharynx and paranasal sinuses can include tumors of the minor salivary glands which line the mucosal surfaces of the nasopharynx and paranasal sinuses.
These would include adenoid cystic carcinomas and mucoepidermoid carcinomas. Adenocarcinomas and rhabdomyosarcomas are also a possibility. Benign tumors would include inverted papilloma which arises from the mucous membranes, but invaginates inwardly into the underlying stroma. The common place for an inverted papilloma to arise would be the lateral nasal wall at the middle meatus. The inverted papilloma is a benign, slow growing lesion, which tends to remottle and enlarge the nasal fossa. It tends to grow inwardly, particularly into the maxillary sinuses, causing obstruction and possibly bone destruction. Epistasis can also be associated with this tumor.
Juvenile nasal angiofibroma
s tend to be seen in teenage males and usually originate along the pterygopalatine
fossa. They are extremely vascular and can follow blood vessels commonly
out to the infratemporal fossa, orbit, and possibly also into the middle
cranial fossa. They can represent with nasal obstruction and epistasis.
One should check for numerous flow voids and widening of the pterytopalatine
foramen.
* Juvenile nasal angiofibroma: * Teenage males. * Epistaxes and/or nasal obstruction. * Arises from pterygopalatine fossa with frequent destruction of pterygoid plates. * Extremely vascular: Check for flow voids on MRI. Do not biopsy unless the tumor has been embolized. * May spread to infratemporal fossa, orbit, skull base. * Low grade malignancy. * Usually slow growing, relentless, and recurrent. * Destroys adjacent architecture by direct invasion. |
* Low grade malignancy. * Slow growing. * Relentless |
* Arises from neuroectodermal cells along cribriform plate, nasal septum, superior turbenates, ethmoid air cells. * Very aggressive and malignant, extends through the cribriform plate and may see the CSF. * A form of PNET like medulloblastoma and pineoblastoma. * May present as cystic mass intracranially. |
1. Harnsberger H, Osborn A. Differential diagnosis of head and neck lesions based on their space of origin. I. The suprahyoid part of the neck. AJR 157:147-154, July 1991.
2. Smoker W, Hansberger H. Differential diagnosis of head and neck lesions based on their space of origin. The infrahyoid portion of the neck. AJR 155:159, July 1991.
3. Hesselink JR, Norbash AM. Nasopharynx and Deep Facial Compartments. in Edelman, Hesselink, Zlatkin & Crues, eds., Clinical Magnetic Resonance Imaging, 3rd edition, Saunders-Elsevier, Philadelphia, 2006, pp 2048-84.
4. Harnsberger HR, Hudgins PA, Wiggins RH, Davidson HC: Diagnostic Imaging – Head and Neck. 1st ed., Saunders, Philadelphia, 2005.
5. Brown J, Chew F. Inverted papilloma. AJR 159:278, August 1992.
6. Som P, Shapiro M. MRI of head and neck. Radiologic Clinics NA, vol. 27, #2, March 1989.
7. Som PM, Curtain HD, eds., Head and Neck Imaging, Mosby-Year Book, St. Louis, 1996, pp. 1300-1549.
8. Buetow P, Smirniotopoulos J, Wenig B. Pediatric sinonasal tumors. Applied Radiology 21-28, February 1993.
9. Drawings adapted from: Harnsberger H, Osborn A. Differential diagnosis of head and neck lesions based on their space of origin. I. The suprahyoid part of the neck. AJR 157:147-154, July 1991.